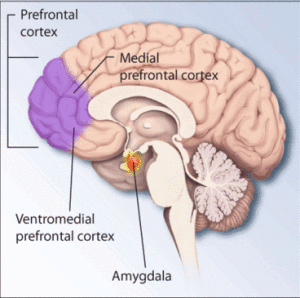
Stress can be caused by sudden physical danger. In evolution, animals developed elaborate mechanisms for rapidly identifying danger and responding with fight or flight responses. When studying humans, it became apparent that the same responses can occur with psychological, interpersonal and work-related stress Further study shows that animals, also, respond to psychological stress in the same ways. Recent research finds responses to stress are much more complex than fight and flight responses. There are a large number of factors that are triggered during different types, intensities and durations of stress. Important regions of the brain, such as the prefrontal cortex, hippocampus, amygdala and hypothalamus all have different elaborate neuroplastic changes with different types of stress and with different intensities and durations. Stress causes many kinds of neuroplasticity in wide-ranging circuits throughout the brain.
Unique Neuroplasticity in the Hypothalamus
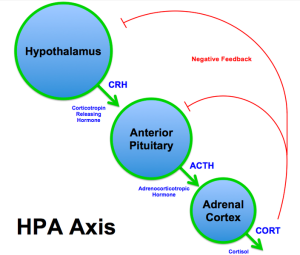
A previous post described unique types of neuroplasticity in the hypothalamus that are not seen elsewhere in the brain. Complex feedback loops of the hypothalamus, pituitary and adrenals make up the HPA axis. which triggers corticosteroids with wide-ranging effects throughout the body. As well, many other factors are involved at the levels of genetic networks. Various neurotrophins (factors that are needed for neuron creation and maintenance) trigger different types of neuroplasticity. The unique neuroplasticity described in the hypothalamus (see previous post) alters all future responses in different time windows—called metaplasticity.
The hypothalamus is the region that registers input from all other parts of the brain about specific types of stress. Regions for emotion, memory, cognition and decision-making all send data to the hypothalamus that then triggers the HPA axis in different ways. Feedback loops regulate the amount of signaling that occurs.
 While unique neuroplasticity occurs in the hypothalamus, the other major parts of the brain—prefrontal cortex, hippocampus, and amygdala—all have very different types of neuroplasticity. These changes have varying effects on the number of dendrites, the shapes of the dendrites, the amount of long-term depression, and many other characteristics. Surprisingly, these changes are quite variable based on the amount and duration of the stress. Even more surprising is that they vary with the types of stress. Neuroplasticity in these three regions impairs cognition while fear and anxiety are increased. From an evolutionary argument, cognition would seem to be as important for animal survival, but is treated differently.
While unique neuroplasticity occurs in the hypothalamus, the other major parts of the brain—prefrontal cortex, hippocampus, and amygdala—all have very different types of neuroplasticity. These changes have varying effects on the number of dendrites, the shapes of the dendrites, the amount of long-term depression, and many other characteristics. Surprisingly, these changes are quite variable based on the amount and duration of the stress. Even more surprising is that they vary with the types of stress. Neuroplasticity in these three regions impairs cognition while fear and anxiety are increased. From an evolutionary argument, cognition would seem to be as important for animal survival, but is treated differently.
The very complex responses to stress are mediated by both the nervous system and the immune systems. All types of perceptions that cause stress—psychological, social and physical—affect both the immune cells and the brain cells at once. Among the many factors that regulate stress responses, cytokines and inflammation play an important role. Previous posts have emphasized that the immune system and the brain are, in fact, one system—the wired and wireless brain. The choroid plexus is the gateway between these two systems that are in constant communication with cytokines and neurotransmitters. T cells in the CFS controlled by the choroid plexus are vital to send signals to the brain to increase cognition under normal circumstances and when sensing infections, sending cytokines to decrease cognition for the sick feelings, which help healing. Neurons can trigger every aspect of inflammation as well.
This post will pick up from the description of the hypothalamus in the previous post to describe the stress related neuroplasticity in these other critical regions.
Stress in Multiple Brain Regions
 Stress stimulates very different brain changes in the important regions of the hippocampus, amydgala and the pre frontal cortex. The hypothalamus integrates information from all over the brain to trigger the well-known HPA stress response. Even one small stress event can have very lasting effects through unique metaplasticity in the hypothalamus.
Stress stimulates very different brain changes in the important regions of the hippocampus, amydgala and the pre frontal cortex. The hypothalamus integrates information from all over the brain to trigger the well-known HPA stress response. Even one small stress event can have very lasting effects through unique metaplasticity in the hypothalamus.
The stress related changes in these regions are, also, critically correlated with psychiatric illness. It has been well known, for example, that stress related psychiatric disorders have a smaller hippocampus associated with a cognitive disorder. The amygdala on the other hand has increased reactivity, not volume changes. The frontal lobes at the same time can have decreased activity.
The three areas have different types of changes at every level of the brain structure including circuits, neurons, synapses, molecules and genetic networks. They each have different effects on the integration of stress in the hypothalamus. As more is learned about the complex interrelationships of these three regions, it is clear that each affects the others in ways that are not yet understood. What is apparent is that each of these brain regions has many ways to control the others. Damaging stimulation that occurs in the amygdala can have severe effects on the two other regions.
Stress Related Neuroplasticity in the Hippocampus
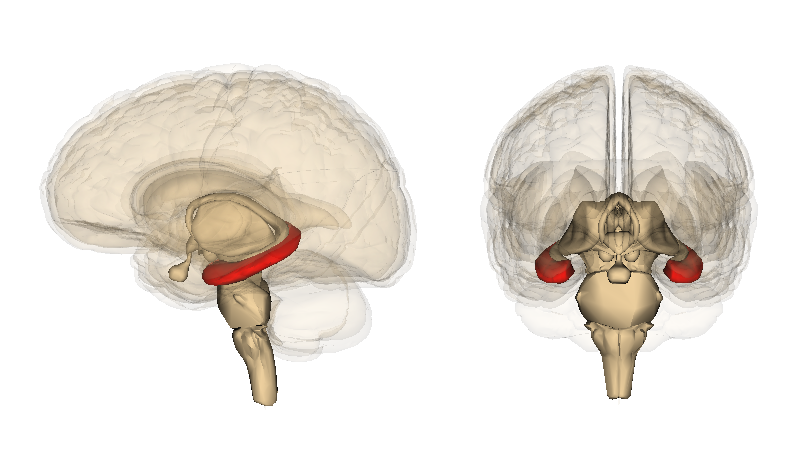
The stress related changes of the hippocampus influence its primary functions such as memory and learning. The hippocampus is critical to important types of memory of time and space, and conscious working memory. The hippocampus is the center for memory that is consciously recalled such as facts and specific verbal learning. This is called either declarative or explicit memory. Declarative refers to memory that can be “declared” in words. Explicit is the type of memory that is recalled with effort—what we think of as “a memory”.
The other type of habit memory (correlated with cerebellum and striatum) is called “non declarative” or procedural and involves the learning of how to do things that do not function as “memory” or in spoken descriptions. The typical example is riding a bicycle.
There are two types of declarative memory that are affected by neuroplasticity changes. One includes personal experiences—an “episode”—called episodic memory, filled with autobiographical events and emotions. The entire experience can be recalled including the situation, context, place and time. The other is remembering facts, called semantic memory. This has been called “knowing” rather than remembering.
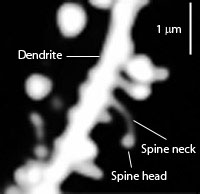
 Neuroplasticity in the hippocampus is highly correlated with cognitive alterations that occur with stress and stress related psychiatric illness. The extensive changes in the dendrite spines include becoming shorter with less branching. These dendrite alterations are related to high levels of glutamate and glucocorticoids in unique patterns.
Neuroplasticity in the hippocampus is highly correlated with cognitive alterations that occur with stress and stress related psychiatric illness. The extensive changes in the dendrite spines include becoming shorter with less branching. These dendrite alterations are related to high levels of glutamate and glucocorticoids in unique patterns.
The loss of volume in the hippocampus appears to be related to atrophy of neurons as well as less newly minted neurons for memory. There appears to be different kinds of neuroplasticity in different region of the hippocampus, but in general there is a change from long term potentiation to the opposite—long term depression. This causes less signaling in general. Factors like BDNF are decreased (a neurotrophin necessary for neuronal function and the creation of new neurons). The hippocampus is one of the regions where stem cells make new neurons each day (around 700 per day) that incorporate themselves in the circuits related to new memories and remodeling of memory. This process is reduced in depression and with long standing stress.
What is surprising is that decreasing the ability to remember may help in a fight and flight mode, but in more complex situations, not remembering correctly can compromise the ability to defend.
The hippocampus is critical for feedback to the HPA axis. The changes that occur can be summarized as:
- A decrease of neural activity
- Decrease of dendrites and spines
- Decreased long term potentiation
- BDNF decreased
- Less neuroplasticity
Stress Related Neuroplasticity in the Medial Pre Frontal Cortex (mPFC)
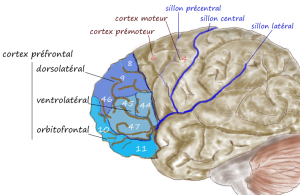 The medial prefrontal cortex is the main/brain region related to decision making and has negative feedback to the HPA related to regulation of the stress response. Like the hippocampus, the pre frontal cortex neuroplasticity is correlated with cognitive changes that occur with stress.
The medial prefrontal cortex is the main/brain region related to decision making and has negative feedback to the HPA related to regulation of the stress response. Like the hippocampus, the pre frontal cortex neuroplasticity is correlated with cognitive changes that occur with stress.
The cortex has many layers and has different complex responses at the each layer and sub region. Each layer is highly connected throughout the brain in different ways. One region has shortening of dendrites in one layer and fewer dendrites and less spines in another. These produce a 40% reduction in synaptic activity. The reduction in these neurons at different layers affects other parts of the brain since the mPFC is vital to regulation of much of the rest of the brain.
Cognition is affected by stress and extreme stress contributes to cognitive disorders, through neuroplasticity of the mPFC. When stress is severe and recurrent, the PFC releases catecholamines that decrease neuronal activity, which decreases cognitive activity. The mechanism involves altering the effectiveness of synapses through the dendrite spines. The weakening occurs through opening in potassium channels (see post on the complexity of potassium channels) from noradrenergic a1 and dopamine D1 receptors.
At the same time these same catecholamines make the sensory cortex more sensitive. They, also, increase activity in the striatum and amygdala. Taken together, these changes in the pre frontal cortex alter behavior from that of analysis and reflective decision to rapid reflex type of behavior. This change to a hyperactive impulsive response occurs as more stress occurs and leads to a long term decrease of the pre frontal cortex function with decreased cognition.
 The changes in the pre frontal cortex can be summarized as:
The changes in the pre frontal cortex can be summarized as:
- Decrease of dendrites and spines
- Decreased long term potentiation
- BDNF increase or decrease
- Messenger RNA increase or decrease
- Weakened connectivity
- Changes from reflective to reflexive
- Disruption making cognitive disorders worse
Stress Related Neuroplasticity in the Amygdala
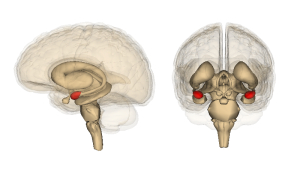 The amygdala has very different types of neuroplasticity than the hippocampus and the pre frontal cortex. Unlike the other two regions, the changes that occur with stress in the amygdala are related to emotional alterations. Both the amygdala and the hippocampus send signals to the hypothalamus stress triggering regions in the PVN. They impact on the GABA neurons differently. The hippocampus and PFC cause excitement and increase GABA activity, which suppresses the HPA. The amygdala does the opposite with decreased inhibition with less GABA and increase of the HPA stimulation.
The amygdala has very different types of neuroplasticity than the hippocampus and the pre frontal cortex. Unlike the other two regions, the changes that occur with stress in the amygdala are related to emotional alterations. Both the amygdala and the hippocampus send signals to the hypothalamus stress triggering regions in the PVN. They impact on the GABA neurons differently. The hippocampus and PFC cause excitement and increase GABA activity, which suppresses the HPA. The amygdala does the opposite with decreased inhibition with less GABA and increase of the HPA stimulation.
Stress causes fear and anxiety and decreases spatial memory. Research into the neuroplasticity of the amygdala is very recent. The earlier work showed that the hippocampus has decreased dendrites with chronic stress. But, in the amygdala (especially the baso-lateral complex BLA) the dendrites grow larger, more numerous and have many more branches. This increase occurs on the excitatory types of neurons (pyramidal and stellate). Stress that is more unpredictable over a long period has less effects in the hippocampus and the amygdala with less anxiety and fearfulness. Steady chronic stress leads to long lasting changes in the amygdala, but reverse occurs in the hippocampus and prefrontal cortex. The remodeling of the BLA causes specific emotional changes.
A summary of the neuroplasticity changes in the amygdala are:
- An increase in neural activity
- Increased dendrites and spines
- Increased long term potentiation
- BDNF is increased
- More neuroplasticity
Different Patterns of Stress Cause Various Neuroplasticity
 Different patterns emerge for different timings of stress. Several hours of stress leads to gradual increase of dendrites but not more arbor branches. After long periods of stress, spine density occurs a day later than the stress and with more arbors. The gradual buildup coincided with gradual increase of anxiety.
Different patterns emerge for different timings of stress. Several hours of stress leads to gradual increase of dendrites but not more arbor branches. After long periods of stress, spine density occurs a day later than the stress and with more arbors. The gradual buildup coincided with gradual increase of anxiety.
Complex paradoxical reactions occur with corticosteroids that are probably related to timing. A large single dose of corticosteroid produces the effects of long lasting stress. Attempts are being made from these animal studies to study PTSD. But, the opposite has been found where people with lower steroids are more likely to develop PTSD. Those treated with steroids in the ICU get less PTSD. Low steroids may avoid starting PTSD, but not PTSD that has already begun. In animals, steroids avoids the development of anxiety in animals. With low steroids and no PTSD, there is no increase of spines. It is the timing of the steroids not the amount that appears to matter.
In the hippocampus, BDNF is critical to help the changes from stress. But, the opposite occurs in the amygdala where increased BDNF increases spines. Chronic stress decreases BDNF in the hippocampus and increases it in the amygdala. The stress dendrites go along with the BDNF.
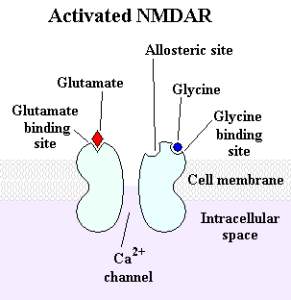 Neuroplastic changes are related to NMDA to AMPA receptors in excitatory neurons. Stress increases the amount of NMDA receptors, which are silent without the AMPA. These are silent synapses (not active), which can makes it more sensitive during future excitation. Chronic stress decreases GABA interneuron effects. Again, the hippocampus and amygdala are opposites in this. But, the effects in the amygdala are so powerful they override the hippocampus.
Neuroplastic changes are related to NMDA to AMPA receptors in excitatory neurons. Stress increases the amount of NMDA receptors, which are silent without the AMPA. These are silent synapses (not active), which can makes it more sensitive during future excitation. Chronic stress decreases GABA interneuron effects. Again, the hippocampus and amygdala are opposites in this. But, the effects in the amygdala are so powerful they override the hippocampus.
Chronic stress breaks down the network between these regions, which causes exaggerations in the alterations. Neuroplasticity between the regions is affected. Each area alters the stress related neuroplasticity of the other regions. The amygdala mediates changes in the hippocampus affecting memory. Brain waves are altered such that the usual memory oscillations between hippocampus regions now went between the hippocampus and the amygdala.
Complex Mechanisms at Many Scales
The more that is learned, the more complex are the factors involved in all the different varieties of stress at different intensities and durations. Many signaling molecules have dramatic influence on this process, including steroid glucocorticoids and excitatory amino acids. But, there are many other factors including endogenous cannabinoids and BDNF (contributes to neuron growth in a positive and negative way). All of these forces trigger genetic networks in complex ways. Stress is now known to trigger epigenetic tagging of histones including CpG methylation and hydroxyl-methylation tags. Also, jumping genes (retrotransposons) in the nucleus DNA have been known to influence genetic activity during stress by causing instability.
 Stress related epigenetic mechanisms are quite complex. Tags alter availability of specific regions of DNA by altering the histones that protect the DNA until it is to be used. As well as the tagging with acetylation, methylation and phosphorylation, there are many other very complex mechanisms. DNA is, also, directly tagged with methyl, hydroxyl methyl groups. Many non-coding RNAs are involved, such as microRNAs and piwi-interacting RNAs, and long non-coding RNAs. These all alter how DNA makes messenger RNAs to make proteins.
Stress related epigenetic mechanisms are quite complex. Tags alter availability of specific regions of DNA by altering the histones that protect the DNA until it is to be used. As well as the tagging with acetylation, methylation and phosphorylation, there are many other very complex mechanisms. DNA is, also, directly tagged with methyl, hydroxyl methyl groups. Many non-coding RNAs are involved, such as microRNAs and piwi-interacting RNAs, and long non-coding RNAs. These all alter how DNA makes messenger RNAs to make proteins.
Among the many new molecules that affect the stress neuroplasticity, two types of adhesion molecules are particularly significant. One of them—neuroligin—is vital to hold synapses together; they project from the pre and post synaptic neurons shaking hands in the middle of the synapse. These are now known to be very important in the balance between excitation and inhibition and in the neuroplasticity of stress.
Stress is a multi-layered process at the genetic, cellular, synaptic levels as well at the social interaction human levels.
Stress Causes Many Kinds of Neuroplasticity
The effects of stress on the brain are extremely complex with many different kinds of neuroplasticity in different brain regions. Different effects occur for individuals (varied resilience) and from various factors of duration, intensity and environment. Stress responses occur in all animals and elaborate mechanisms have evolved to deal with physical, emotional and social stress. These mechanisms involve changing genetic networks and epigenetic tags on DNA and histones and many different factors and hormones. Even a brief exposure can have lasting effects.
It is mental events that trigger these vast complex changes in genetic networks, neurons, synapses and circuits. Different perceptions of psychological and interpersonal problems, along with the awareness of physical illness and danger trigger these vast changes in physical structures at eight orders of magnitude and scale. Further research will gradually understand how these different mental events can instantly and over time alter molecules, neurons and brains.

